Collapsed Trachea in Small Dogs: Signs, Triggers, and Treatment Options
If you’ve ever been in a room with a Chihuahua or Pomeranian having a coughing fit that sounds more like a goose honking than a cough, you’ve probably witnessed a collapsed trachea episode. It’s startling the first time, and understandably alarming. The trachea, the airway connecting the throat to the lungs, is supported by cartilage rings that keep it open during breathing. In some small and toy breeds, those rings are softer and less rigid than they should be, and under certain conditions the airway partially collapses, producing that distinctive honking cough.
Alpine Animal Hospital in Pocatello provides comprehensive care for small breeds throughout the region, with the diagnostic tools and treatment options needed to manage tracheal collapse properly. Same-day evaluation through our urgent care is available when symptoms flare, and you can schedule an appointment at any time to have your dog’s airway evaluated.
What Collapsed Trachea Is and How It Develops
The trachea is essentially a flexible tube held open by C-shaped cartilage rings, with a soft membrane closing the back of the C. When that cartilage weakens, the tube flattens during breathing, especially on inspiration, and air has to squeeze through a much narrower passage. That narrowing produces the cough.
Tracheal collapse is a progressive condition, meaning it tends to worsen gradually over time rather than appearing all at once. It’s most common in middle-aged to senior small and toy breeds, with Yorkies, Pomeranians, Chihuahuas, Shih Tzus, Pugs, and Maltese topping the list. Genetic cartilage weakness is the underlying cause for most affected dogs, but several factors can speed the progression: obesity, chronic coughing from any source, frequent collar use, secondhand smoke, and environmental irritants. Our small animal services cover the full picture for these breeds, from puppy visits through senior care, and we’re happy to talk through harness choice and environmental modifications to prevent tracheal collapse from worsening.
Severity Grades and What They Mean
Tracheal collapse is graded by how much the airway narrows during breathing, and the grade often guides treatment decisions:
| Grade | Airway Narrowing | Typical Symptoms | Common Approach |
| Grade 1 | Up to 25% | Occasional honking cough with excitement | Lifestyle adjustments, monitoring |
| Grade 2 | 25-50% | More frequent cough, mild exercise intolerance | Medical management |
| Grade 3 | 50-75% | Daily cough, breathing effort during episodes | Aggressive medical management; stenting considered |
| Grade 4 | 75% or near-complete | Severe respiratory distress, episodes interfering with rest | Stenting often discussed |
What Are the Symptoms of Collapsed Trachea?
The hallmark sign is the honking cough, sometimes described as goose-like or seal-like. It tends to appear during or right after specific triggers:
- Excitement, especially greetings and play
- Pulling against a collar
- Drinking water (often followed by gagging)
- Hot or humid weather
- Cold air, particularly during Pocatello winters when the air is dry and harsh
- Eating, especially dry food
Beyond the signature cough, you might notice:
- Exercise intolerance, with shorter tolerance for walks or play
- Faster or more laboured breathing
- Restlessness or difficulty settling
- Episodes triggered by stress
- Worsening at night
Symptoms range from mild and occasional to severe and frequent, and they often progress over months to years rather than days. If your small dog’s coughing is changing, becoming more frequent, or starting to come with breathing effort, our urgent care services can usually evaluate the same day.
Emergency Warning Signs That Need Immediate Care
There’s a meaningful difference between chronic management and an acute crisis. Most coughing episodes in a dog with collapsed trachea resolve in a few minutes once the trigger is removed. A true respiratory emergency does not. Come in right away for any of the following:
- Severe difficulty breathing at rest, with visible heaving of the chest or belly
- Cyanosis (blue, gray, or muddy gum or tongue color, indicating poor oxygen delivery)
- Collapse, severe weakness, or loss of consciousness
- Inability to catch breath even after several minutes of calm
- A cough that does not stop and seems to interfere with breathing itself
Any of these signs is a true pet emergency. Emergency stabilization for severe airway distress typically involves oxygen therapy, sedation to break the panic-cough-panic cycle that worsens collapse, and medications to reduce airway inflammation and bronchospasm. Once the immediate crisis is controlled, we can plan longer-term management.
Diagnosing Collapsed Trachea
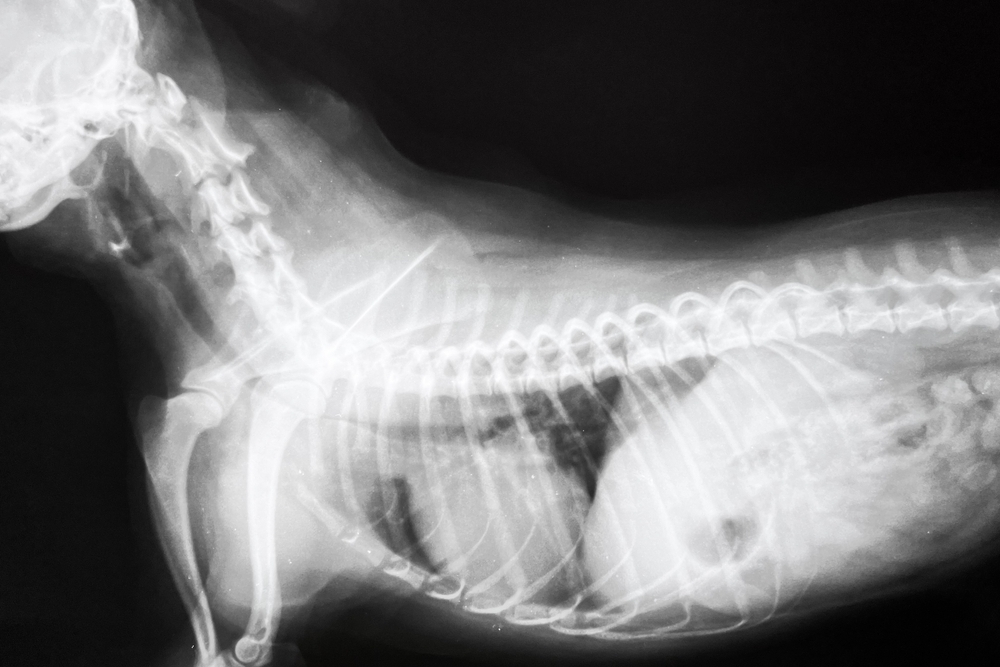
Diagnosis begins with a thorough physical exam, including listening carefully to the lungs and trachea while the dog breathes and gently coughs. Most pets with tracheal collapse will cough when the trachea is gently palpated. Other conditions can mimic collapse and need to be ruled out: heart disease, chronic bronchitis, laryngeal paralysis, kennel cough, and pneumonia all cause coughing that can sound similar to a worried family. Many cases of mild to moderate collapse can be confirmed with a combination of breed signalment, characteristic cough, and chest radiographs taken during inspiration and expiration. The trachea looks dramatically different on the two views when collapse is present.
Alongside the well-known small breeds, brachycephalic breeds (Pugs, Bulldogs, Frenchies) often have similar symptoms and multiple airway issues stacked together. Brachycephalic airway syndrome sometimes has a component known as “hypoplastic trachea“, where the trachea is simply too narrow and can be hard to differentiate from tracheal collapse without proper diagnostics.
For more nuanced cases, fluoroscopy (a real-time, moving X-ray) shows the trachea collapsing during the respiratory cycle and grades the severity from mild (Grade 1\) to nearly complete (Grade 4). Tracheoscopy, which uses a tiny camera placed into the airway under sedation, allows direct visualization. Both typically require referral to a specialist. Our team takes the time to work through the differential list carefully so the treatment plan actually fits the diagnosis, and will explain every step of the diagnostic process.
Medical Management for Mild to Moderate Cases
Most dogs with collapsed trachea can be managed well with medication and lifestyle adjustments alone. The medical toolkit typically includes:
- Cough suppressants (such as hydrocodone or butorphanol) to break the cough-irritation cycle
- Anti-inflammatories, often corticosteroids in short courses, to reduce airway swelling
- Cerenia, used off-label (it’s typically used for nausea and vomiting), can be helpful for some patients
- Bronchodilators to relax the airway smooth muscle and improve airflow
- Antibiotics, only when secondary infection is documented
- Sedatives for short-term use during predictable triggers like travel or storms
- Laser therapy, which can help decrease inflammation and reduce coughing for some patients
Medications are tailored to your dog’s specific symptoms and severity, and they often need adjustment over time as the condition progresses. Consistent follow-up matters; we like to recheck dogs on chronic medication every 3 to 6 months to make sure the plan is still working and to catch progression early.
When Is Surgery or Stenting the Right Call?
For dogs with severe collapse (Grade 3 or 4) that does not respond adequately to medical management, tracheal stent placement can be life-changing. A stent is a flexible mesh tube placed inside the trachea to support the cartilage from within. The procedure is minimally invasive and is typically done by a board-certified specialist with the right imaging equipment.
Stenting is not a cure. Most stented dogs still need ongoing medical management, and there are risks worth understanding:
- Stent fracture over time
- Displacement within the airway
- Granulation tissue formation at the stent edges
- Persistent or recurrent coughing
That said, for dogs with severe symptoms that significantly limit their quality of life, the benefits often outweigh the risks. Surgical correction of the trachea itself (using external prosthetic rings) is another option, typically reserved for younger dogs with cervical (neck-region) collapse rather than intrathoracic (chest-region) collapse. Case selection matters enormously, and we work with you to weigh whether referral for advanced intervention makes sense for your dog.
Modifiable Triggers and Daily Comfort
The good news is that many risk factors are modifiable, and the daily habits that reduce flare-ups are the same ones that keep already-diagnosed dogs comfortable long-term. The biggest wins come from small, consistent changes:
- Switch to a harness, always. Pressure on the throat from a collar (especially during pulling) directly aggravates collapse. A harness takes pressure off the throat and distributes it across the chest and shoulders. This single switch reduces flare-ups for almost every dog with tracheal collapse and is non-negotiable.
- Manage weight closely. Even a pound or two of extra weight on a small dog adds noticeable load to breathing. Weight loss is one of the single most effective interventions for many tracheal collapse patients. Talk with us about target weight and a realistic feeding plan.
- Avoid environmental irritants. Cigarette smoke, scented candles, aerosol cleaners, harsh cleaning products, and heavy fragrances all worsen airway inflammation.
- Keep the home calm and cool during summer, and avoid hot midday walks.
- Use a humidifier during dry winter months to keep airways from drying out further. Pocatello winters are notably hard on small airways.
- Stay current on vaccinations. Bouts of kennel cough or other respiratory infections cause coughing fits that can accelerate cartilage damage. Keeping up with vaccinations, including DHPP (that last “P” stands for parainfluenza), Bordetella, and Canine Influenza helps reduce that risk.
- Address dental disease. Untreated dental disease increases pneumonia risk, since these dogs cannot breathe as effectively and run a higher chance of inhaling bacteria from their mouths.
- Break exercise into shorter sessions rather than one long walk.
- Keep calm during coughing fits. Excitement worsens the cycle.
- Consider anti-anxiety medications or sedatives during times you know your pet will become overly excited, like holidays or fireworks.
- Monitor breathing patterns at rest. Knowing your dog’s resting respiratory rate (count breaths per minute when they’re sleeping) makes it easy to spot a real change. Normal is 30 breaths per minute or less; borderline is 30 to 40; 40 or higher is a strong signal that they should be seen promptly.
If something feels off and you’re not sure whether it’s a flare-up or something more, reach out to us and we’ll walk you through it.
Long-Term Prognosis and Quality of Life
Here’s the reassuring part: most dogs with collapsed trachea live happy, comfortable lives for years with the right management plan. The condition is progressive, but the rate of progression is highly variable, and proactive care meaningfully slows it down for many dogs.
Severity at diagnosis is the strongest predictor of long-term outlook. Dogs caught in mild stages and managed proactively often do very well for the rest of their lives. Dogs presenting with severe collapse have a more complicated path but can still respond beautifully to a combination of medication, lifestyle changes, and stenting when appropriate.
For chronic management, our advanced services include Class 4 laser therapy, which can reduce airway and soft tissue inflammation as part of an overall comfort plan. Senior dogs with collapsed trachea often benefit from the same approach used for arthritis and other chronic conditions: a multi-modal plan that addresses inflammation, comfort, and overall vitality from several directions at once.
Frequently Asked Questions About Collapsed Trachea in Dogs
Is collapsed trachea painful for my dog?
The collapse itself is not particularly painful, but the coughing fits are uncomfortable, exhausting, and can cause genuine distress, similar to how a long coughing fit feels for a person. Severe episodes that interfere with breathing are very stressful for the dog. Good management keeps those episodes infrequent and brief.
Can collapsed trachea be cured?
No, but it can be managed very effectively. The cartilage damage doesn’t reverse, but symptoms can be controlled with medication, lifestyle changes, and, in severe cases, stenting.
Will my dog grow out of it?
Unfortunately no. Tracheal collapse tends to develop gradually and progress over time rather than improve. The good news is that progression is often slow, and most dogs maintain a good quality of life for years.
Is it safe for my small dog to wear a collar at all?
A collar for ID and a leash quick-attach is fine, but the leash itself should always attach to a harness. Pulling against a collar is one of the most consistent triggers we see for flare-ups.
When should I consider stent surgery for my dog?
When medical management is no longer adequately controlling symptoms and quality of life is meaningfully reduced. We can talk through where your dog falls on that spectrum and whether referral makes sense at the moment.
Partnering With Us for Easier Breathing
Collapsed trachea sounds scary the first time you hear that cough, but the reality is that with the right care plan, most dogs with this condition live full, comfortable lives. Early diagnosis, consistent medical management, lifestyle changes that take pressure off the airway, and a clear plan for what to do during a flare-up together cover the vast majority of cases.
Whether you’re concerned about a new cough, looking for a second opinion on chronic management, or wondering if stenting is the right move for a dog who’s been struggling, our team is here to help. Schedule an appointment for a respiratory evaluation or contact us with questions. Alpine Animal Hospital provides veterinary care in Pocatello across the full range of what your dog needs, from wellness to urgent care even after our doors are closed. Your dog’s comfort matters, and we’re here to make breathing easier for them, and for you.





Leave A Comment